Diagnostic Tests for Fertility Assessment


At C.M.R, we offer a comprehensive range of diagnostic tests dedicated to fertility assessment, aimed at both women and men. Thanks to advanced technologies and a team of qualified specialists, it is possible to identify potential causes of infertility and plan the most appropriate treatment.
Among the available tests, we include gynecological and andrological visits, specific ultrasounds, hormonal tests, semen analysis, and innovative techniques such as sonohysterosalpingography and hysteroscopy. Each procedure is designed to ensure maximum comfort and diagnostic accuracy, guiding couples through a personalized and professional journey.
Trust our experience to face every stage of the diagnosis with peace of mind and find the solutions best suited to your needs.

It initially consists of a bimanual examination to assess any conditions affecting the external (vulva and vagina) and internal (uterus, ovaries) genital organs, followed by a speculum examination for visual assessment of the cervix.
The visit can be complemented by a transvaginal ultrasound to evaluate the presence or suspicion of conditions such as fibroids, endometrial polyps, or ovarian cysts.
The visit and ultrasound are not painful.
If requested, a PAP TEST can be performed at the center, which allows screening for the prevention of neoplastic lesions of the cervix.
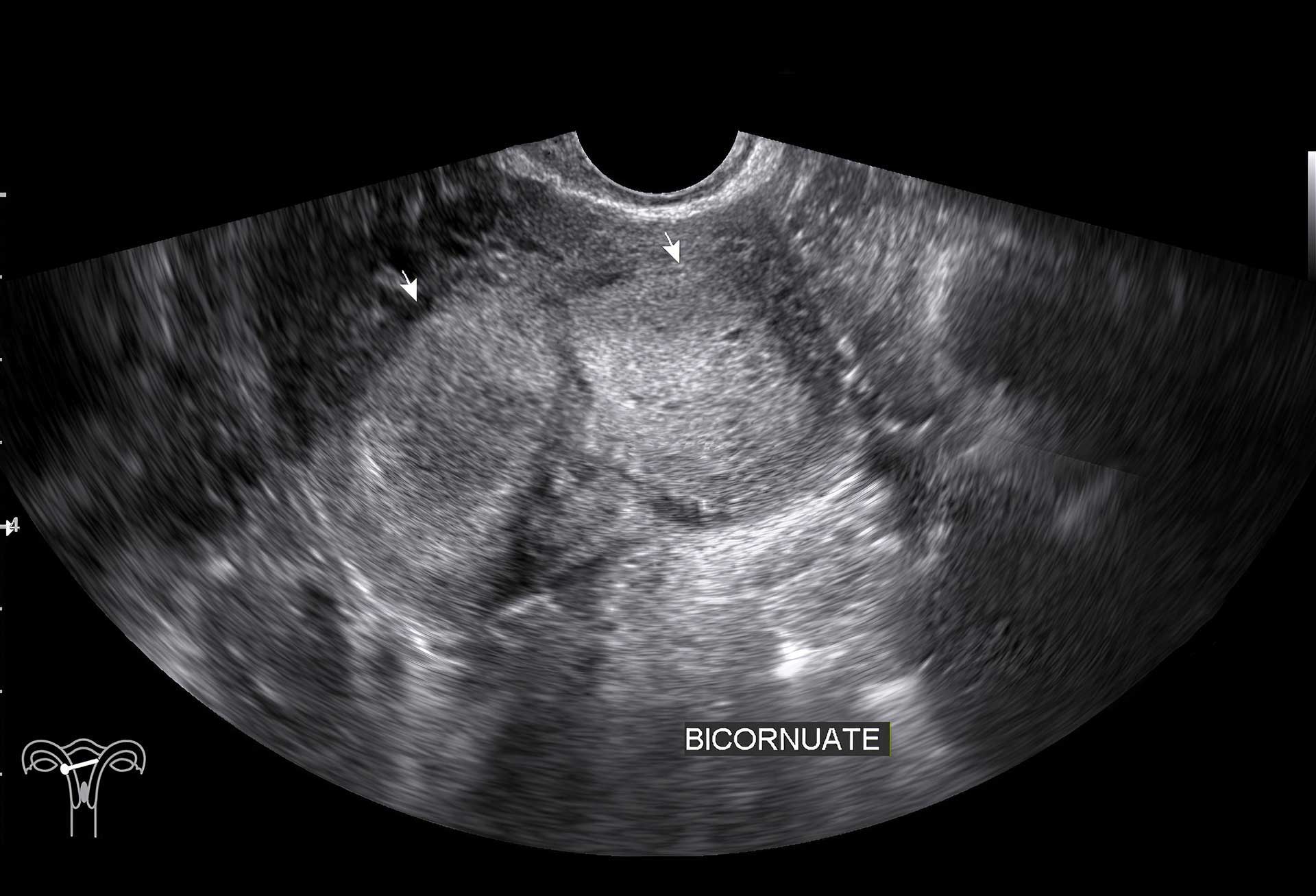
This method uses ultrasound emitted by a probe placed on the abdomen (transabdominal ultrasound) or inserted into the vagina (transvaginal ultrasound) to visualize the internal genital organs, uterus, ovaries, and tubes, the latter being visible only if pathologically dilated (hydrosalpinx/salpingitis).
The goal is to visualize the morphology of these organs and identify any atypical masses or malformations.
This examination is not painful and poses no risks as it does not use ionizing radiation but harmless ultrasound waves.
This is an ultrasound method that allows for the assessment of tubal patency and the identification and/or exclusion of alterations in the uterine cavity.
It involves the introduction, through a small catheter inserted vaginally, of 10-20 cc of saline solution and air into the uterine cavity, with the subsequent passage (or non-passage) of the same through the tubes into the peritoneal cavity.
The examination must be performed by the 12th day of the menstrual cycle.
This type of diagnostic exam allows for the evaluation, through a 3D ultrasound, of the inside of the uterine cavity and the possible presence of related pathologies.
It is performed when a malformation or the presence of polyps, fibroids, or adhesions (synechiae) is suspected.
The procedure is carried out in an outpatient setting and is painless.

The ovarian cycle, whether natural or pharmacologically stimulated, is monitored with serial ultrasounds of follicular and endometrial growth, up to the moment of ovulation.
This ultrasound monitoring is often associated with hormonal monitoring of estradiol production and possibly other hormones involved in the ovulation mechanism.

This type of diagnostic exam allows for the evaluation of the uterine cavity and the possible presence of related pathologies through 3D ultrasound.
It is performed when a malformation or the presence of polyps, fibroids, or adhesions (synechiae) is suspected.
The procedure is carried out in an outpatient setting and is painless.

This is an endoscopic method that allows for the diagnosis and potential treatment of various pathological conditions affecting the uterus (cervix and body).
It is performed by introducing a thin fiber-optic instrument through the cervical canal. In over 95-97% of cases, the exam can be performed on an outpatient basis.
Hysteroscopy allows for the diagnosis of uterine malformations and the possible presence of adhesions, polyps, fibroids, and tumors of the uterus. During the examination, tissue samples can be taken for histological analysis.

This is a visit aimed at evaluating male fertility, which allows for the non-invasive and painless identification of any anatomical anomalies, alterations caused by infectious or traumatic processes, or monitoring the progress of previously diagnosed conditions for which the patient is undergoing treatment.
A couple undergoing a diagnostic process for infertility must consider performing a spermogram, which is an examination conducted on a semen sample obtained through masturbation and properly collected in a sterile container for urine.
To perform the examination, a period of abstinence from sexual intercourse (ejaculations) of between 2 and 6 days is required.
Our center is equipped with suitable rooms for semen collection.
In extraordinary cases, it is possible to collect semen at home, but it is strictly necessary to deliver the sample to the laboratory no later than 40 minutes after collection and to avoid drastic temperature changes (20-37 °C).
Initially, the spermogram analyzes macroscopic parameters such as the total volume, appearance, and odor of the sample, pH, degree of liquefaction and viscosity, and the potential presence of round cells.
It is possible to complete the analysis by performing a sperm culture.

This fertility evaluation analysis is performed on a semen sample and aims to investigate the potential presence of microbiological populations responsible for inflammatory processes affecting the genital tract.
In some cases, they may be the cause of unsuccessful fertilization.

This is a test that involves evaluating the number of "best" sperm in terms of morphology and motility by removing seminal plasma through washing, separating them from dead sperm and debris.
This type of test, as its name indicates, aims to detect breaks or lesions in the genetic material of the sperm.
DNA fragmentation in sperm can be caused by alterations in the spermatogenesis process, excessive production of reactive oxygen species in the ejaculate, exposure to environmental or industrial toxins, oxidative stress, and smoking. All these are well-known causes that lead to DNA fragmentation and infertility.
The percentage of sperm with fragmented DNA is detected using the TUNEL method (Terminal deoxynucleotidyl transferase dUTP Nick End Labeling), which involves the use of enzymes capable of identifying the presence of breakpoints in the DNA double helix.
A semen sample with a percentage of sperm with fragmented DNA greater than 30% is considered pathological.

This test involves the search for anti-sperm autoantibodies, which can sometimes bind to the surface of sperm, inhibiting their functionality and interfering with the fertilization process.
This screening test allows for the identification of the significant presence of two main classes of immunoglobulins (IgA and IgG) bound to the surface of the sperm.
This examination consists of an aspiration biopsy of sperm using a needle that penetrates the skin, which is performed when sperm cannot be found in the semen.
The procedure is necessary when the male partner presents with azoospermia (i.e., absence of sperm in the ejaculate) due to an obstruction of the seminal pathways.
Sometimes, sperm may be found in the testicle or epididymis, although in very small numbers.
The FISH test (Fluorescence In Situ Hybridization) is a molecular biology technique used to detect specific DNA or RNA sequences in cells or tissues.
It uses fluorescent probes that bind to complementary sequences, allowing visualization of their location.
In the context of Assisted Reproductive Technology (ART), the FISH Test is applied to the analysis of sperm. It represents the study of chromosomes in sperm using fluorescent probes. This test allows us to identify whether the chromosomal composition of the sperm is normal or not.
The FISH Test is a useful tool for generating higher quality embryos.

The staff at CMR is here to support you through the activation of an ONLINE CONSULTATION desk, where they will answer all your questions to establish a first approach and begin an important journey together.